Healthcare Providers And Systems Brace For A Third Recovery Wave, 6,100 Monthly Cancer Patients, And 2.5 Million Elective Patient Gap
Tuesday 1st February
As far as intensity goes, this has been one of the most extreme and challenging Februarys in history for the healthcare sector. As a I write this, we are simultaneously experiencing one of the most transformative periods in healthcare, while systems in the UK and across the globe continue to struggle in delivering urgent and routine services.
The volumes of patients waiting for high, medium and low risk procedures or care continue to grow at an accelerated rate, backlogs of cancer cases already exceeding 104 days with over 6,100 patients this month, compared to 3,000 last year. Within the rapidly growing national surgical waiting list, there are approximately 103,491 patients requiring treatment within four weeks in the face of a significant risk of deterioration.
Professor Neil Mortensen, president of England’s Royal College of Surgeons, said the growing backlogs were “very worrying”, adding: “My focus at the start of 2021 has been trying to support surgeons to find ways to keep urgent surgery going through these challenging times.”
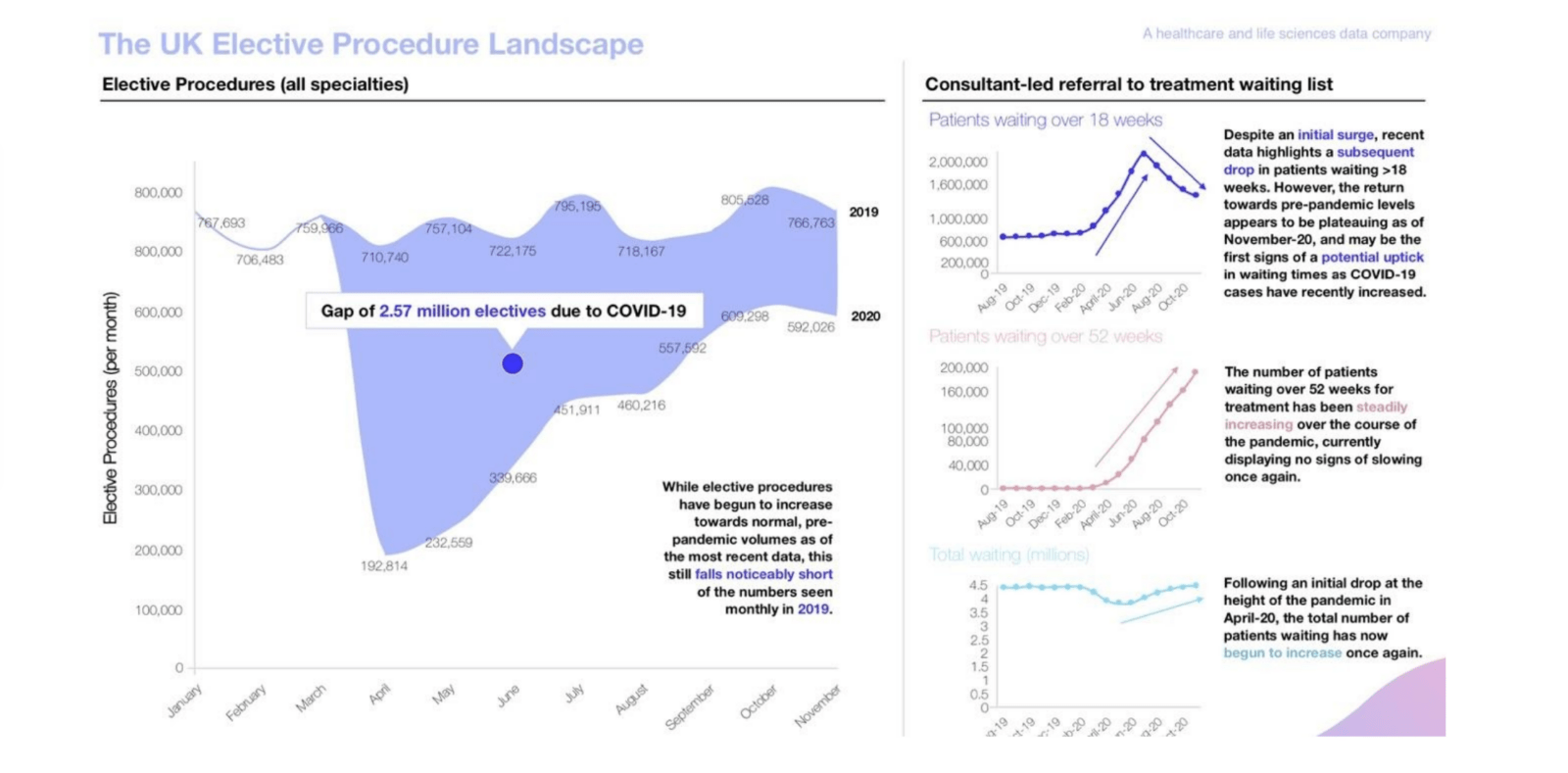
Our advanced analytics, powered by RwHealth’s health Data Science Platform (DSP), highlights a 2.5m gap (shown below) which needs to be closed for elective patients alone. Despite these challenging times, clinical and leadership teams are taking the opportunity to accelerate new ways of working as they plan for a tight window of recovery before the next wave of Covid-19, flu and other disruptive viruses over the coming year.
As we approach an anticipated easing of lockdown measures and head into the spring, our modelling and predictive analytics emphasise the need for frontline clinical teams to take well deserved breaks. While absolutely essential, this will in turn potentially temporarily slow down the backlog recovery effort. When compounded with the harsh reality that the real barriers to recovery aren’t purely the number of Covid-19 cases, but a more deeply ingrained set of issues – namely a shortage of 58% within the healthcare workforce, 44% in bed capacity and 28% in operating room capacity – I believe that this is something we can all relate to, as capacity has now become a real issue for many.
Once again reflecting on the words of Professor Neil Mortensen, the truth is that many “NHS staff are burnt out” from the experience of working without a break through Christmas and the New Year, right on the back of a hellish year where many were unable to deliver the standards of care to their patients that they first entered into their professions to provide. There is no point to politicians talking about operating 24/7 in order to get the NHS back on track when many anaesthetists, theatre staff and surgeons will need time to recuperate come Spring. There are now national plans being discussed for some sort of break for NHS staff, and although the precise shape this will take is not yet decided, it will surely be very welcome.
To learn more about the current elective landscape, insights for recovery, and predictive analytics for the NHS’s upcoming demand surges, download our detailed report via the form here.
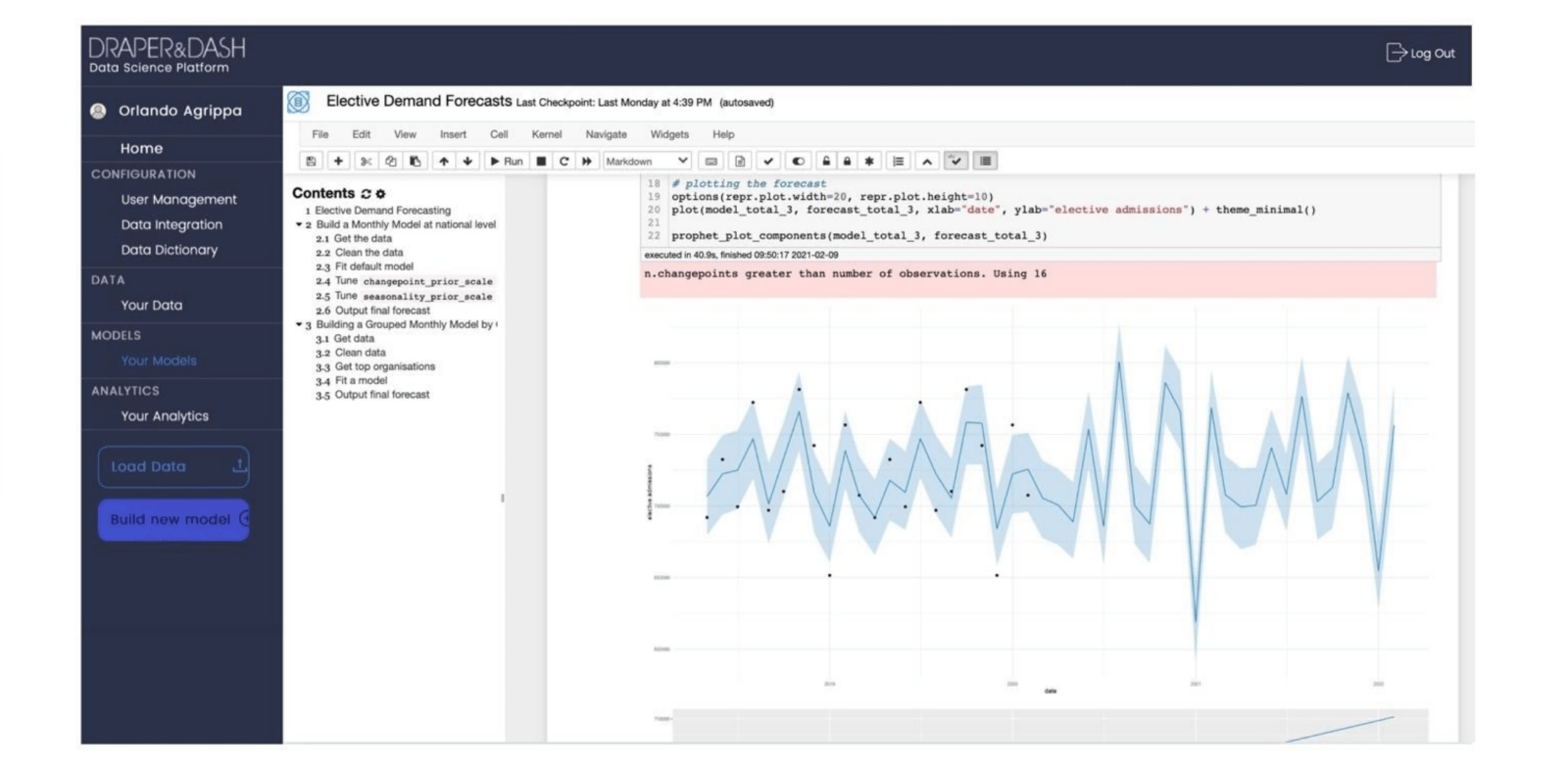
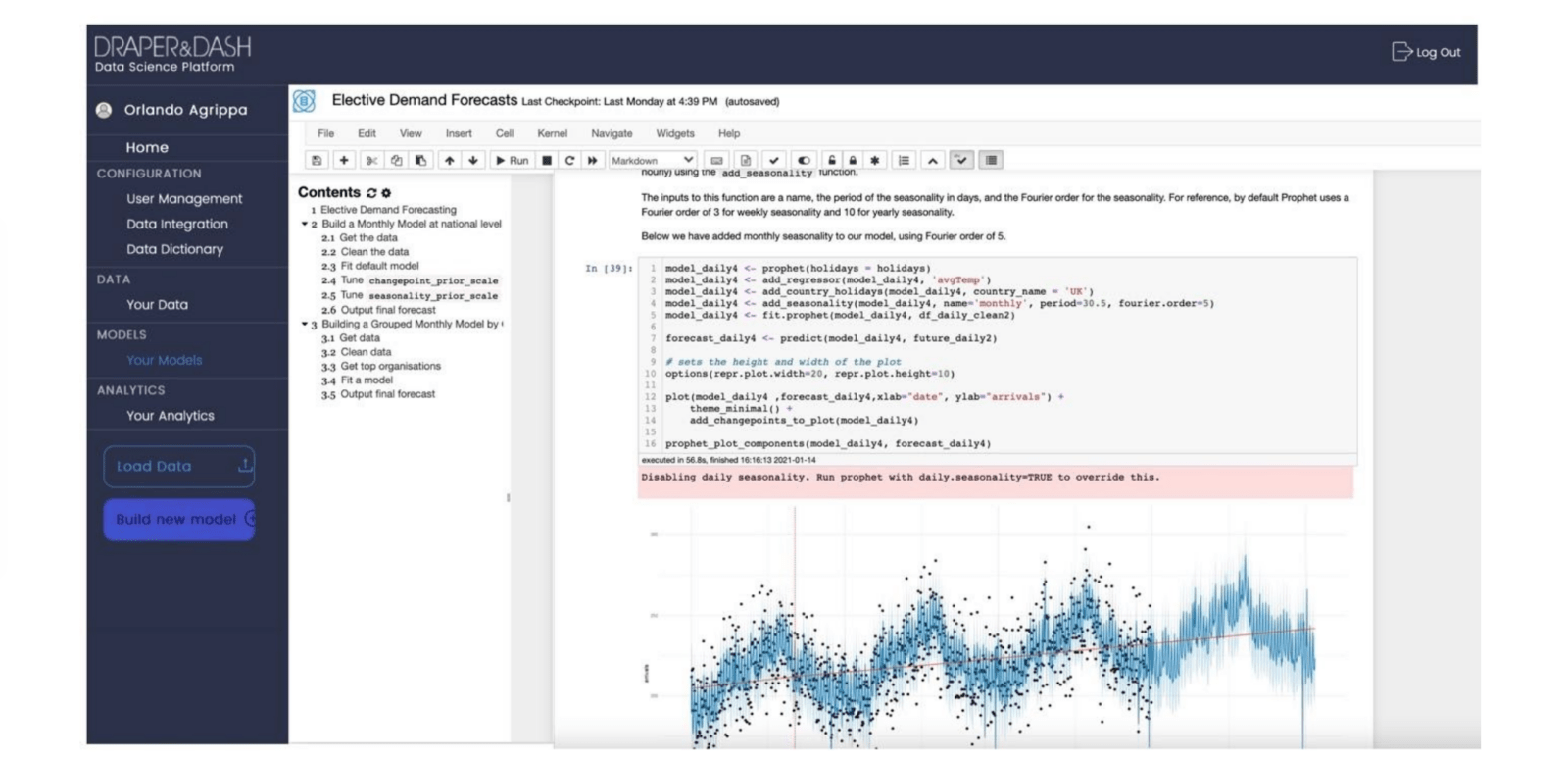
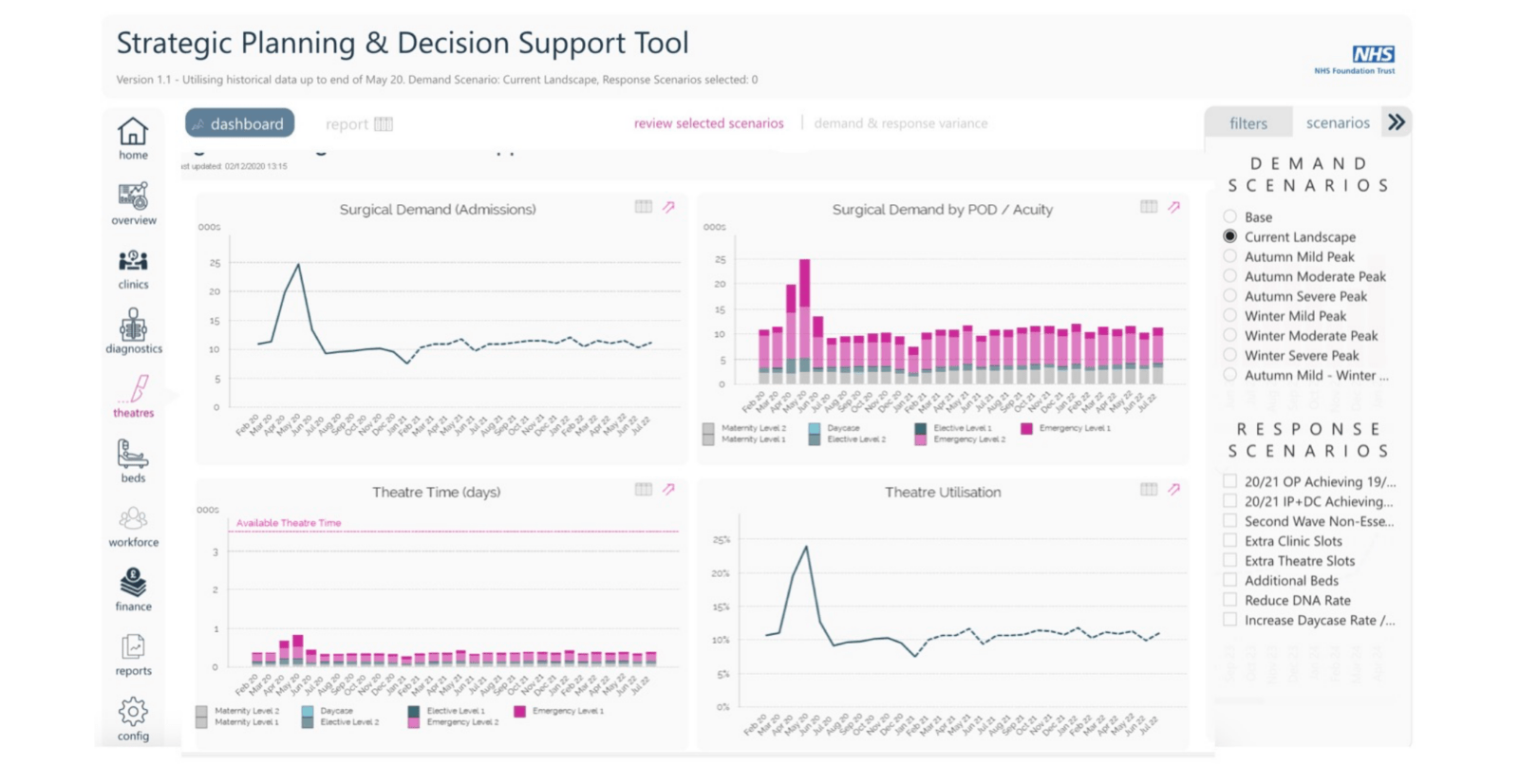
We have been working with a number of providers and systems, both nationally and internationally, to support with leveraging advanced predictive machine learning and data science for the modelling of targeted scenarios. These support areas including:
- New elective pathway mapping and new ways of working.
- Profiling the waiting list and patent risk stratification at both a local and system level.
- New ways of addressing the capacity gap.
- Supporting workforce shortages by optimising new models of care.
- Modelling patient complexity and admission criteria.
- Predicting the Summer demand and Autumn/Winter surges, with stand-up and stand down models.